When a doctor suspects something is wrong with your liver, kidneys, uterus, or any organ tucked inside your abdomen or pelvis, an ultrasound sonography test is usually the first imaging tool they reach for. It’s fast, painless, radiation-free, and delivers real-time pictures of your internal organs within minutes. Whether your physician has ordered an abdominal scan, a pelvic scan, or a combined USG A+P test, understanding what the procedure involves takes away most of the anxiety around it.
This guide covers everything you need to know about the USG test: what it is, why doctors order it, how to prepare, what the results mean, and what risks (if any) to expect.
What Is an Ultrasound Scan Test (USG) — Abdominal / Pelvic?
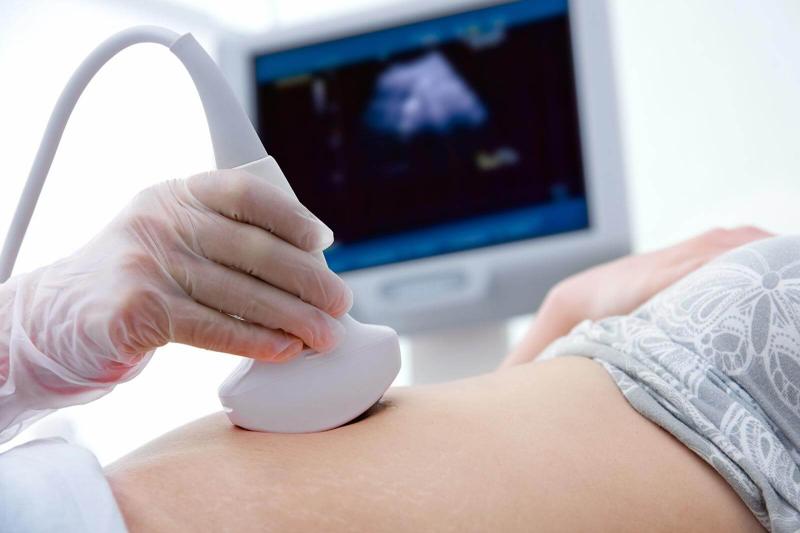
USG full form is Ultrasonography, sometimes written as Ultrasound Sonography. The USG test uses high-frequency sound waves, typically between 2 and 18 megahertz, to create real-time images of the structures inside your body. A small handheld device called a transducer emits these sound waves and picks up the echoes that bounce back from organs, tissues, and fluids. A computer then converts those echoes into the images your radiologist reads on screen.
An abdominal USG focuses on the organs in your upper and lower abdomen: the liver, gallbladder, spleen, pancreas, kidneys, aorta, and the surrounding lymph nodes. A pelvic USG focuses on the bladder, uterus, ovaries, fallopian tubes (in women), and the prostate gland and seminal vesicles (in men). When both regions need to be evaluated together, the combined procedure is ordered as a USG A+P test, meaning abdominal and pelvic ultrasound in a single sitting.
It is worth distinguishing a USG from a USD test. While these terms are sometimes confused informally, a USD test in a clinical context usually refers to an upper segment defect scan or is simply a regional shorthand. Your requisition form will almost always specify “USG Abdomen,” “USG Pelvis,” or “USG A+P.” If your form says something different, ask your doctor to clarify.
The technology itself is the same as the sonography test used in obstetrics to monitor pregnancy, but the clinical purpose and scanning technique differ based on which organ system is being examined.
Why Do I Need an Ultrasound Sonography Test?
Doctors order a USG test when they need to see the size, shape, texture, and position of your internal organs without exposing you to radiation. Unlike a CT scan or X-ray, ultrasound uses no ionizing radiation, which makes it the preferred first-line imaging choice for a wide range of clinical concerns, including those affecting pregnant women, children, and patients who need repeated monitoring.
Your physician may order a USG test if you report symptoms such as unexplained abdominal pain, bloating, nausea, urinary problems, menstrual irregularities, or if routine blood work shows abnormal liver, kidney, or pancreatic enzyme levels. The sonography test helps bridge the gap between what a physical examination can detect and what requires more invasive investigation.
Because the procedure is quick, affordable, portable, and widely available, it is often the starting point for clinical decision-making. In many cases, a USG test is all a physician needs to confirm or rule out a diagnosis. In others, it narrows the diagnostic possibilities enough to guide the next step, whether that is a blood test, an MRI, a CT scan, or a biopsy.
Reasons to Take an Ultrasound Sonography Test (USG) — Abdominal / Pelvic
The clinical indications for a USG test are broad. Below are the most common reasons physicians request this scan.
Abdominal indications:
Fatty liver disease (hepatic steatosis) is one of the most frequent diagnoses made on an abdominal USG test. The scan assesses liver echogenicity, size, and surface texture, giving the radiologist enough information to grade the severity of fat accumulation. Gallstones are another major indication. Even stones as small as 2 to 3 mm can be detected on a sonography test, along with gallbladder wall thickening and bile duct dilation that suggest obstruction.
Kidney-related problems such as renal cysts, hydronephrosis (fluid backup caused by a blockage), kidney stones, and changes in renal parenchyma (the functional tissue of the kidney) are clearly visible on USG. The pancreas is harder to visualize due to its location behind the stomach, but when bowel gas is minimal, the scan can detect pancreatic masses, pseudocysts, and ductal dilation. Splenic enlargement (splenomegaly), often associated with liver disease, infections, or blood disorders, is also assessed routinely during an abdominal USG.
Free fluid in the abdominal cavity, known as ascites, appears clearly on ultrasound as anechoic (fluid-dark) areas between the loops of bowel and around the organs. This is a critical finding in patients with liver cirrhosis, heart failure, or malignancy.
Pelvic indications:
In women, a pelvic USG is ordered to evaluate the uterus and ovaries. The scan detects fibroids (benign uterine tumors), ovarian cysts, polycystic ovary syndrome (PCOS), endometrial thickening, and ovarian masses. It is also the primary scan used to confirm intrauterine pregnancy and monitor early fetal development in the first trimester.
In men, a pelvic USG evaluates the bladder for wall thickening, diverticula, and post-void residual volume. The prostate is assessed for enlargement (benign prostatic hyperplasia or BPH) and irregular nodules that may warrant further investigation.
Combined USG A+P Test:
When symptoms are not clearly localized to either the abdomen or the pelvis, or when a systemic condition such as cancer, tuberculosis, or lymphoma needs to be staged across both regions, the USG A+P test is ordered. This single session covers the entire abdominal and pelvic cavity and gives the treating physician a comprehensive anatomical overview in one report.
Preparations Needed for Ultrasound Sonography Test (USG) — Abdominal / Pelvic
Preparation makes a measurable difference in image quality. A poorly prepared patient, particularly one with a full stomach or empty bladder at the wrong time, can result in suboptimal images that obscure findings or require a repeat scan.
For an abdominal USG:
You are typically required to fast for 6 to 8 hours before the scan. The reason is straightforward: when you eat, the stomach fills with food and gas, and the gallbladder contracts to release bile. A contracted gallbladder is harder to assess, and bowel gas scatters sound waves, reducing image quality significantly. Fasting keeps the gallbladder distended and the bowel relatively gas-free, giving the sonographer a clear acoustic window.
You may drink plain water during the fasting period. Avoid carbonated drinks, milk, and juices. Some facilities ask you to avoid even water for a shorter window of 2 to 3 hours before the scan. Follow the specific instructions your diagnostic centre provides.
For a pelvic USG:
A full urinary bladder is required for a transabdominal pelvic sonography test. The bladder, when full, acts as a natural acoustic window, pushing the gas-filled bowel out of the way and allowing the transducer to get clear images of the uterus, ovaries, and prostate beneath it.
You will typically be asked to drink about 4 to 6 glasses of water (roughly 1 litre) one hour before the scan and to avoid urinating until after the procedure. Arrive with a comfortably full bladder, not so full that you are in pain, but full enough that the radiologist can use it as a landmark.
For a combined USG A+P test:
Preparation combines both requirements: fast for 6 to 8 hours for the abdominal portion and ensure a full bladder for the pelvic portion. Drink water about an hour before the appointment so the bladder fills during the fasting window.
Additional general preparations:
Wear loose, two-piece clothing that allows easy access to your abdomen and lower pelvis without needing to undress entirely. Inform the technician or physician if you have had previous abdominal surgeries, are pregnant, or have known allergies to ultrasound gel (rare but worth mentioning). Remove any jewellery or belts around the abdominal area.
Sample Required?
No blood sample, tissue sample, or any biological specimen is required for a USG test. Ultrasound sonography is a non-invasive imaging procedure. The only things needed are your presence, the appropriate preparation (fasting or a full bladder as specified), and the ultrasound gel applied to your skin, which serves as a coupling medium between the transducer and your body.
However, your doctor may order a USG test alongside blood tests (such as liver function tests, renal function tests, or a complete blood count) to correlate imaging findings with laboratory data. In those cases, a blood draw happens separately, either before or after your scan, and is not part of the USG procedure itself.
What Other Tests Might I Have Along with an Ultrasound Sonography Test?
A USG test rarely stands alone in a diagnostic workup. It is most often ordered alongside or followed by additional investigations based on what the scan reveals.
Blood tests: Liver function tests (LFT), kidney function tests (KFT/RFT), serum amylase and lipase (for pancreatic conditions), complete blood count (CBC), and tumour markers such as CA-125 (for ovarian pathology) or AFP (for liver masses) are frequently paired with an abdominal or pelvic USG.
Urine tests: A urine routine and microscopy examination is often ordered alongside a renal or pelvic USG to check for infection, blood in the urine (haematuria), or proteinuria.
CT Scan or MRI: If the USG test detects a mass, a complex cyst, or a finding that needs better characterization, a CT scan (which gives cross-sectional images with high anatomical detail) or an MRI (which offers superior soft-tissue contrast without radiation) will be ordered as the next imaging step. USG findings guide which modality is most appropriate and which body region to focus on.
Endoscopy: If an abdominal USG points toward pathology in the upper gastrointestinal tract (oesophagus, stomach, or duodenum) or biliary system, an upper GI endoscopy or ERCP (endoscopic retrograde cholangiopancreatography) may follow.
Colour Doppler USG: This is a variant of the standard sonography test that assesses blood flow within organs and vessels. It is frequently ordered alongside a routine abdominal USG to evaluate portal hypertension, hepatic vein thrombosis (Budd-Chiari syndrome), renal artery stenosis, or ovarian torsion.
Biopsy: When a USG detects a solid liver lesion, a renal mass, or a suspicious pelvic nodule, an ultrasound-guided biopsy may be performed. The USG acts as a real-time guide for the needle, making the biopsy more precise and safer.
What Do My USG Test Results Mean?
USG results are interpreted by a radiologist and communicated to your treating physician in a written report, typically available within a few hours to 24 hours after the scan. Here is what common findings mean in practical terms.
Normal findings: The report will describe each organ’s size, echogenicity (brightness level on screen), contour, and internal texture as normal. For example, a normal liver report might read: “liver is normal in size and echotexture, no focal lesion seen.” A normal pelvic report in a woman might state: “uterus is anteverted, normal in size and echotexture; both ovaries are normal.”
Fatty liver (hepatic steatosis): Described as increased hepatic echogenicity (the liver appears brighter than normal on screen). Graded as mild, moderate, or severe based on the degree of brightness and whether deeper structures are obscured.
Gallstones (cholelithiasis): Appear as echogenic foci (bright spots) within the gallbladder that cast an acoustic shadow (a dark streak beneath the stone). The number, size, and location of stones are documented.
Renal calculi (kidney stones): Similar to gallstones, kidney stones appear as echogenic foci with posterior acoustic shadowing in the collecting system of the kidney.
Cysts: Simple cysts are anechoic (completely dark inside), round or oval, with thin walls and posterior acoustic enhancement (the area behind the cyst appears brighter). Complex cysts with internal echoes, septations, or thick walls require further evaluation.
Fibroids: Appear as hypoechoic (darker than surrounding tissue) or heterogeneous masses in or around the uterine wall, with varying sizes and locations (subserosal, intramural, or submucosal).
PCOS: The ovaries appear enlarged, with multiple small follicles arranged peripherally (the classic “string of pearls” appearance), and an increased ovarian volume above 10 cc.
Free fluid / Ascites: Appears as anechoic areas between the bowel loops, around the liver (Morison’s pouch), or in the pelvis (pouch of Douglas).
If your report contains any of these findings, do not interpret them in isolation. Always discuss results with your treating physician, who will correlate the USG findings with your symptoms, blood tests, and clinical history before making a diagnosis or recommending treatment.
How Is the Ultrasound Sonography Test Done?
The procedure takes between 20 and 45 minutes depending on whether it is an abdominal scan, a pelvic scan, or a combined USG A+P test. Here is a step-by-step breakdown of what happens.
Step 1: Registration and preparation check. You check in at the diagnostic centre, and a technician confirms your preparation (fasting status and bladder fullness). You will be asked to change into a gown or pull up your clothing to expose the relevant area.
Step 2: Positioning. You lie down on an examination table, usually on your back (supine position). For certain views, especially of the kidneys and spleen, the technician may ask you to turn onto your left or right side.
Step 3: Gel application. A water-based, odourless, and hypoallergenic gel is applied to your skin over the area to be scanned. This gel eliminates air pockets between the transducer and your skin, which would otherwise block the sound waves.
Step 4: Scanning. The sonographer moves the transducer firmly but gently over your skin in different directions and at different angles. You may be asked to hold your breath briefly during the scan of certain organs, particularly the liver and spleen, because respiratory movement can blur the image. The transducer sends sound waves inward, and the echoes return and are displayed as a real-time moving image on the monitor.
Step 5: Image capture and measurement. The sonographer captures still images and takes measurements of organ dimensions, cyst sizes, stone diameters, and any abnormal structures. These measurements are recorded in the report.
Step 6: Post-scan. The gel is wiped off your skin. You may resume eating and drinking immediately if you were fasting. If you have been holding your bladder, you can use the restroom right after the pelvic portion is completed.
Step 7: Report generation. A radiologist reviews the images and measurements and prepares a written report. Depending on the facility, this may be available the same day or the following day.
Does the Ultrasound Sonography Test Pose Any Risk?
No, a standard USG test carries no known risks when used for diagnostic imaging. Ultrasound uses non-ionizing sound waves, not radiation. There is no cumulative exposure concern, no contrast injection in a standard abdominal or pelvic sonography test, and no needles or incisions involved.
The gel used on the skin is hypoallergenic and unlikely to cause reactions. It is water-soluble and wipes off easily after the procedure.
Because ultrasound is radiation-free, it is the preferred imaging test for pregnant women, young children, and patients who need repeated monitoring over time, such as those with chronic liver disease or recurring ovarian cysts.
The only potential discomfort is mild pressure from the transducer on the skin, and for a pelvic scan, the mild discomfort of maintaining a full bladder. Neither constitutes a risk in the clinical sense.
There is one important caveat: while ultrasound is safe, an incorrectly interpreted result can lead to unnecessary anxiety or missed diagnoses. This is why your images must be reviewed by a qualified radiologist, and the report must be discussed with your treating physician in the context of your full clinical picture.
What Might Affect My Test Results?
Several factors can reduce image quality or make specific organs difficult to visualize, affecting the accuracy and completeness of the USG report.
Bowel gas: Gas in the intestines is the most common obstacle in abdominal USG. Sound waves cannot pass through gas and are reflected back, creating a “shadow” that obscures organs behind it. This is why fasting before an abdominal scan is so important. In some patients, particularly those with chronic bloating or irritable bowel syndrome, residual gas even after fasting can limit the pancreatic view.
Obesity: A thicker abdominal wall attenuates (weakens) sound waves before they reach deep organs. Higher-frequency transducers that produce sharper images have less penetration depth. In significantly obese patients, a lower-frequency transducer is used, which has greater depth penetration but somewhat lower image resolution.
Recent barium studies or colonoscopy: Barium used in radiographic studies coats the bowel wall and reflects ultrasound heavily. If you have had a barium enema or barium swallow recently, inform your radiologist, as residual barium significantly degrades USG image quality.
An empty or partially full bladder during pelvic USG: The bladder serves as the acoustic window for pelvic imaging. If it is not full enough, the uterus, ovaries, and prostate may be poorly visualized or appear displaced.
Patient cooperation and breathing: Involuntary movement, breathing irregularly, or inability to hold the breath as instructed reduces image sharpness. This is most relevant in young children or anxious patients.
Previous surgeries and scar tissue: Adhesions and surgical scars on the abdominal wall can alter organ positions and create acoustic artefacts (false signals) that complicate interpretation.
Operator experience: Ultrasound is a highly operator-dependent imaging modality. A skilled, experienced sonographer can obtain diagnostic-quality images in challenging patients. The quality of your scan is directly linked to the training and experience of the person performing it.
How Do I Prepare for the Test?
To summarize the preparation concisely:
For abdominal USG:
- Fast for 6 to 8 hours before the test. You may drink plain water.
- Avoid carbonated drinks, milk, tea, coffee, and food.
- Arrive on time. A late scan after eating defeats the preparation purpose.
- Inform the centre if you are diabetic and rely on fasting-sensitive medication, so they can advise appropriately.
For pelvic USG:
- Drink 1 litre of water (4 to 6 glasses) about 1 hour before the test.
- Do not urinate after drinking until after the scan is completed.
- Arrive with a comfortably full bladder.
For a combined USG A+P test:
- Fast for 6 to 8 hours AND maintain a full bladder.
- Drink water within the fasting window so your bladder fills naturally while you have not eaten.
On the day of the test:
- Wear comfortable, loose-fitting clothes.
- Inform the sonographer about any recent surgeries, prior imaging, or if you are pregnant.
- Carry your doctor’s requisition form and any prior scan reports or blood test results.
At-Home USG Test: Top Locations
Home-based diagnostic services now offer USG tests in major Indian cities. Qualified sonographers visit the patient’s home with a portable ultrasound machine and conduct the scan in a comfortable, familiar environment, which is particularly beneficial for elderly patients, bedridden individuals, or those who find commuting to a diagnostic centre difficult.
Home USG services are available in cities including:
- Delhi / NCR (New Delhi, Gurgaon, Noida, Faridabad, Ghaziabad)
- Mumbai (including Navi Mumbai and Thane)
- Bengaluru
- Chennai
- Hyderabad
- Pune
- Kolkata
- Ahmedabad
- Jaipur
- Lucknow
- Chandigarh
- Kochi
When booking a home USG test, verify that the service provider employs DMRD- or MD-qualified radiologists to read the images, uses well-maintained portable equipment that meets diagnostic-grade standards, and delivers a formal written report signed by a registered radiologist.
Conclusion
An ultrasound sonography test is one of the most versatile and patient-friendly diagnostic tools available. Whether you are getting a USG A+P test to investigate a complex symptom, a standalone abdominal USG to check your liver and kidneys, or a pelvic sonography test to evaluate reproductive health, the procedure is safe, quick, and genuinely informative.
The key to getting the most out of your USG test is preparation: fasting correctly for abdominal scans, maintaining the right bladder fullness for pelvic scans, and going to a reputable centre staffed by trained sonographers and qualified radiologists. The scan itself is the easy part. What matters is who reads it and how the findings are used to guide your care.
If your doctor has ordered a USG test, follow the preparation instructions carefully, keep your appointment, and bring all relevant medical records. A single scan, properly done and properly read, can answer questions that might otherwise take weeks of guesswork to resolve.
Frequently Asked Questions
1. What is the USG full form in medical terms?
USG full form is Ultrasonography. In everyday clinical language, it is also called an ultrasound scan or sonography test. It uses high-frequency sound waves to produce real-time images of internal organs and structures.
2. Is a USG test the same as a sonography test?
Yes. The terms USG test and sonography test refer to the same procedure. Both use ultrasound technology to image internal organs. The names are interchangeable in clinical and laboratory contexts across India and most of South Asia.
3. What does a USG A+P test cover?
A USG A+P test covers both the abdominal and pelvic regions in a single scan session. Abdominal coverage includes the liver, gallbladder, spleen, pancreas, kidneys, and aorta. Pelvic coverage includes the bladder, uterus, ovaries (in women), and prostate (in men).
4. How long does a USG test take?
A standard abdominal or pelvic USG test takes about 20 to 30 minutes. A combined USG A+P test may take 30 to 45 minutes. Complex cases requiring detailed assessment of multiple structures may take slightly longer.
5. Is the ultrasound sonography test painful?
No, the USG test is painless. The only sensation is mild pressure from the transducer on your skin. For a pelvic scan, the discomfort of maintaining a full bladder beforehand is the most common complaint, but this resolves immediately after the scan when you can use the restroom.
6. Can I eat before a pelvic USG if I am not having an abdominal scan?
If you are having only a pelvic USG (and not an abdominal scan), fasting is usually not required. The preparation requirement is a full bladder. However, always confirm with your diagnostic centre, as some facilities may have specific protocols.
7. What is the difference between a USD test and a USG test?
These terms are sometimes confused. USG refers to ultrasonography, which is the standard imaging procedure described throughout this article. USD in a clinical context may refer to upper segment defect or is used informally in some regional settings. If your prescription says “USD test,” confirm with your doctor what is meant to avoid attending the wrong examination.
8. Can children undergo a USG test?
Yes. Because ultrasound uses no radiation, it is safe for infants, children, and adolescents. It is frequently used to evaluate abdominal pain, kidney anomalies, and pelvic conditions in paediatric patients. The preparation requirements are the same but adjusted for the child’s age and size.
9. How soon will I get my USG test results?
Most diagnostic centres provide USG reports within 1 to 4 hours of the scan. Some facilities offer same-day reporting; others may take up to 24 hours, particularly if a radiologist needs to review complex images or consult a specialist. Home-based services typically send digital reports by email or WhatsApp within a few hours.
10. Does a USG test detect cancer?
An ultrasound sonography test can detect masses, irregular growths, and abnormal tissue changes that may suggest malignancy. However, USG alone cannot confirm a diagnosis of cancer. If a suspicious lesion is found, further imaging (CT scan or MRI) and a tissue biopsy are required for definitive diagnosis.